Plan Your Visit
Hours
Mon–Thur: 8am – 7pm
Friday: 8am – 5pm
Saturday: 8am – 12pm
Sunday: Closed
Phone
After-Hours Immediate Care: (316) 261-8825
Fax
Clinical Fax: (866) 514-0974
Dental Fax: (888) 662-7106
COVID-19 is an infectious disease caused by a newly discovered coronavirus. COVID-19 was identified in December 2019 and is caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), a new virus in humans causing respiratory illness which can be spread from person-to-person.
According to the World Health Organization, many people infected with the COVID-19 virus will experience mild to moderate respiratory illness and recover without requiring special treatment. However, older people, and those with underlying medical problems like cardiovascular disease, diabetes, chronic respiratory disease, and cancer are more likely to develop serious illness.
Looking for something specific? Click the links below to browse directly to a section on this COVID-19 resource page.
The Sedgwick County Health Department (SCHD) now has an online COVID-19 data dashboard on the Sedgwick County website. It features data from when the first case presented itself on March 6 to present time.
The dashboard is updated daily and includes the number of COVID-19 cases, recoveries, deaths, hospitalizations, illness onset, and cases identified by gender, ethnicity, and race. It allows residents to stay updated on the virus by combining all statistics in one location.

COVID-19 is primarily transmitted from person-to-person through respiratory droplets. These droplets are released when someone with COVID-19 sneezes, coughs, or talks. Infectious droplets can land in the mouths or noses of people who are nearby or possibly be inhaled into the lungs. We recommend maintaining social distancing practices such as people staying 6-feet apart.
Respiratory droplets can land on hands, objects, or surfaces around people when a person coughs or talks. People can then become infected with COVID-19 from touching hands, objects, or surfaces with droplets and then touching their eyes, nose, or mouth.
There can be transmission of COVID-19 through droplets of those with mild symptoms or those who do not feel ill (asymptomatic).
The best way to prevent and slow the transmission of COVID-19 is to be well informed about the virus, the disease it causes, and how it spreads. Protect yourself and others from infection by washing your hands or using an alcohol-based rub frequently and not touching your face.

A wide range of symptoms for COVID-19 has been reported. These include:
The severity of symptoms varies from mild to severe. Early data says that most patients will recover spontaneously with some supportive care. Severe cases have resulted in respiratory failure, septic shock, and/or multiple organ dysfunction or failure, and death.
The estimated incubation period according to the CDC is between 2 and 14 days. It is important to note that some people become infected and do not develop any symptoms or feel unwell (asymptomatic).
If you have symptoms of COVID-19, please call us first at 316-691-0249. Do not walk-in, we will screen you over the phone first and walk-ins will not be allowed. Once you have been screened over the phone, you may be scheduled into our respiratory clinic to meet with a member of our respiratory team. Your provider may have you take a Covid-19 test and will provide you information and instructions on how to properly quarantine and address your symptoms. If you are in an emergency, please call 9-1-1.
Researchers say anywhere from 25 percent to 80 percent of people with COVID-19 are unaware they have the virus. This is called being “asymptomatic,” having no symptoms. People who are asymptomatic can still spread the virus to others who will be symptomatic. This large percentage of asymptomatic people allows the coronavirus to spread more rapidly throughout a community. This is why it is imperative that people wear face masks in public.
If you are asymptomatic and fear you have come in contact with the COVID-19 virus, you should self-quarantine immediately. Quarantine helps prevent spread of disease that can occur before a person knows they are sick or if they are infected with the virus without feeling symptoms. People in quarantine should stay home, separate themselves from others, monitor their health, and follow directions from their state or local health department.
It is important to note that COVID-19 is a new disease, therefore there is limited information regarding risk factors for severe disease. In some cases, people who get COVID-19 can become seriously ill and develop difficulty breathing. These severe complications can lead to death. The risk of severe disease increases steadily as people age. Additionally, those of all ages with underlying medical conditions (including but not limited to heart disease, diabetes, or lung disease) appear to be at higher risk in developing severe COVID-19 compared to those without these conditions. As more data become available, additional risk factors for severe COVID-19 may be identified.

There are a number of ways to prevent the spread of COVID-19 infection. These include the following everyday activities:

Looking for protection from COVID? Here are some Coronavirus facts to help you protect against COVID.
Wearing a mask or face-covering helps protect those around you.
Masks are a simple barrier to help prevent your respiratory droplets from reaching others. Studies show that masks reduce the spray of droplets when worn over the nose and mouth. You should wear a mask, even if you do not feel sick. The main function of wearing a mask is to protect those around you, in case you are infected but not showing symptoms.

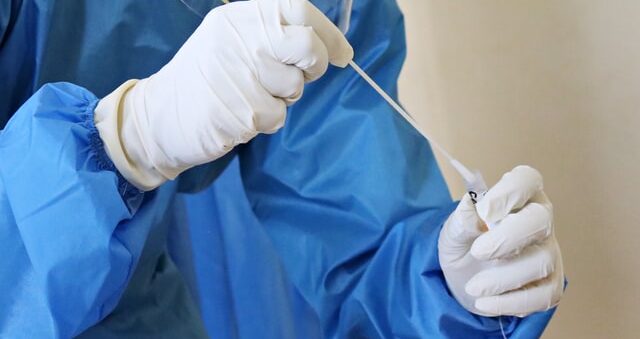
If you have symptoms of COVID-19, your health provider may advise a COVID test. A diagnostic COVID-19 test can show if you have an active coronavirus infection and should take steps to quarantine or isolate yourself from others. Currently, there are two types of diagnostic tests: Molecular tests, such as RT-PCR tests, that detect the virus’s genetic material, and antigen tests that detect specific proteins from the virus. A COVID-19 test involves gathering a saliva sample by either nasal or throat swab.
If you test positive for COVID-19 (coronavirus), you should isolate yourself for 10 days after your symptoms began and ensure you have not had a fever for at least 3 days without the use of fever-reducing medication, and have had improving symptoms for 3 days.
If you test positive for COVID-19, close contacts need to quarantine for 10 days from their last contact with you. This duration of quarantine may be decreased to 7 days under certain conditions when tested negative at least 5 days from the last contact. If the positive case is a household member, the quarantine starts at the end of the positive patient’s isolation. Close contacts are anyone who lives in the same household or anyone who has spent more than 10 minutes within 6 feet of someone diagnosed with COVID-19. The contact includes up to 2 days prior to the onset of the positive person’s symptoms. This close contact quarantine is only for patients who do not develop symptoms. If a close contact does develop symptoms, they must quarantine for 14 days.
If you live with a person of increased risk of severe illness, take added precautions at home to protect that individual according to CDC guidelines.
If you test negative, your healthcare provider may still ask you to self-isolate under certain circumstances.
If your symptoms worsen while self-isolating, contact your healthcare provider immediately. Moderate to severe symptoms may include shortness of breath or severe fatigue. If you are in an emergency, please call 9-1-1.
HealthCore Clinic has a respiratory clinic where we conduct drive-through and walk-up COVID testing. Please call us first at 316-691-0249. Do not walk-in, we will screen you over the phone first and walk-ins will not be allowed. Once you have been screened over the phone, you may be scheduled to meet with a member of our respiratory team. Your provider may test you for COVID-19 and will provide you information and instructions on how to properly quarantine and address your symptoms. If you are in an emergency, please call 9-1-1.
Because some of the symptoms of flu and COVID-19 are similar, it may be hard to tell the difference between them based on symptoms alone, and testing may be needed to help confirm a diagnosis.

Currently, care for patients with COVID-19 is primarily supportive. Care is given to patients to help relieve symptoms and manage respiratory and other organ failures. There are currently no specific antiviral treatments licensed for COVID-19, however many treatments are under investigation. Remdesivir, which is also an investigational drug, received Food and Drug Administration (FDA) emergency use authorization for the treatment of hospitalized patients.
The federal government has been working since the start of the pandemic to make COVID-19 vaccines available as soon as possible. HealthCore Clinic, and other community health centers, are COVID-19 vaccination sites for Wichita.
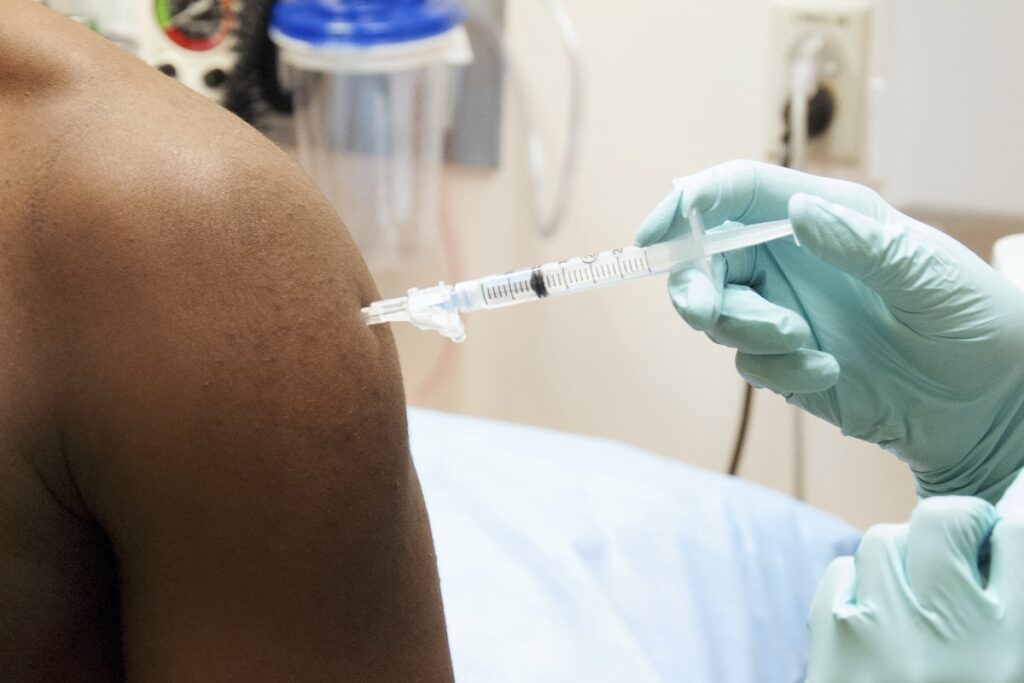
Both the Pfizer Vaccine and Moderna Vaccine have shown essentially equivalent degrees of efficacy to reduce the risk of severe Covid disease. Despite similar production technologies, Pfizer and Moderna’s vaccines have differences such efficacy, storage protocols, and availability. Both vaccines use mRNA technology to trigger an immune response instead of putting a weakened or inactivated germ into the body. The mRNA COVID-19 vaccines teach our cells how to make a protein—or even just a piece of a protein—that triggers an immune response inside our bodies. That immune response, which produces antibodies, is what protects us from getting infected if the real virus enters our bodies.
The Johnson & Johnson vaccine has an efficacy of 66% and only requires a single dose. This vaccine is based on the COVID-19 virus’s genetic instructions for building what’s called a “spike protein.” Unlike the Pfizer and Moderna vaccines, which store the instructions in single-stranded RNA, the Johnson & Johnson vaccine uses double-stranded DNA.
To learn more about the vaccines, visit our Vaccine Comparison Guide.
These side effects usually start within a day or two of getting the vaccine. They might feel like flu symptoms that typically go away in a few days.

COVID-19 vaccines have been tested in large clinical trials to assess their safety. It does take time, and more people getting vaccinated before we learn about very rare or long-term side effects. That is why safety monitoring will continue with organizations such as the CDC.
Most people do not have serious problems after being vaccinated. Your arm may be sore, red, or warm to the touch. These symptoms usually go away on their own within a week. Some people report getting a headache or fever when getting a vaccine. These side effects are a sign that your immune system is doing exactly what it is supposed to do. It is working and building up protection against the disease.
Both this disease and the vaccine are new. We don’t know how long protection lasts for those who get infected or those who are vaccinated. What we do know is that COVID-19 has caused very serious illness and death for a lot of people. If you get COVID-19, you also risk giving it to loved ones who may get very sick. Getting a COVID-19 vaccine is a safer choice.
To receive the COVID-19 Vaccine from HealthCore Clinic you must meet the following requirements.
HealthCore Clinic has taken multiple steps to increase safety at our clinic including the development of a dedicated respiratory clinic, adding safety partitions, increased PPE, added risk assessments, increased preventative action, teleheath options, drive-thru/walk-up COVID-19 testing by appointment, and increased cleaning and sterilization of the facility as outlined by the CDC.
A mask or similar face covering is required to enter HealthCore Clinic and everyone will be screened at the door before being allowed to enter. There are exceptions to the face-covering requirement such as…
You will be allowed to remove your face-covering when receiving health attention involving the nose or face for which temporary removal of the face-covering is necessary to perform the service.
Mon–Thur: 8am – 7pm
Friday: 8am – 5pm
Saturday: 8am – 12pm
Sunday: Closed
After-Hours Immediate Care: (316) 261-8825
Clinical Fax: (866) 514-0974
Dental Fax: (888) 662-7106
Look for emergency warning signs* for COVID-19. If someone is showing any of these signs, seek emergency medical care immediately:
*This list is not all possible symptoms. Please call your medical provider for any other symptoms that are severe or concerning to you.
Call 911 or call ahead to your local emergency facility: Notify the operator that you are seeking care for someone who has or may have COVID-19.